Let’s Stop Violence against Healthcare Professionals
{“dynamic”:true,”content”:”post_excerpt”,”settings”:{“before”:””,”after”:””,”words”:”10″,”read_more_label”:””}}
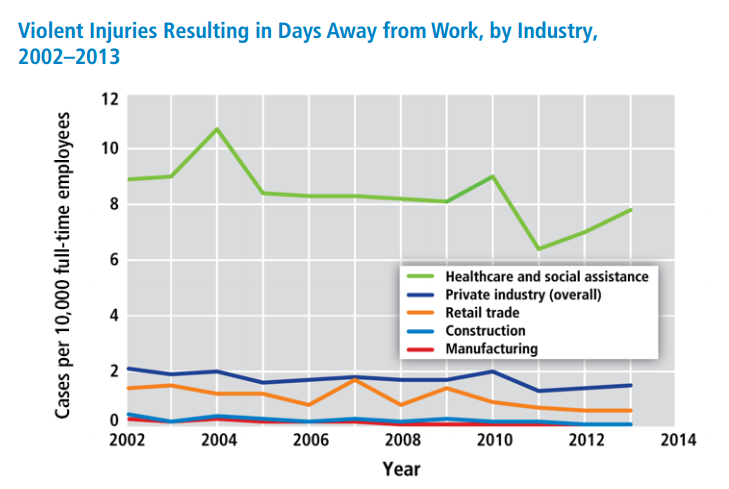
From 2002 to 2013, incidents of serious workplace violence (those requiring days off for the injured worker to recuperate) were four times more common in healthcare than in private industry on average. In 2013, the broad “healthcare and social assistance” sector had 7.8 cases of serious workplace violence per 10,000 full-time employees (see graph below). Other large sectors such as construction, manufacturing, and retail all had fewer than two cases per 10,000 full-time employees.
- Too-early release of injured and unstable patients due to insurance guidelines
- Available narcotics in hospital settings attract addicts
- Fights between patients and between patients’ families (if the victims of a street fight are transported to the E.D., and both sides of the fight end up in the same hospital, the fight might continue there)Frustration at hospital and insurance policies
- Understaffing
- It must be dramatically reduced. Those who care for others deserve a safe workplace.
- After-action reports are critical learning tools. Who is causing harm, where in the facility, and when? Precise knowledge helps define safety improvements.
- Train all employees to diffuse violent situations, report threats, and defend themselves, their colleagues and their patients.
- Regularly exercise plans, policies, and procedures aimed at reducing assaults, and improve them after each exercise.
0 Comments
Related Articles: CMS Rules for Healthcare Providers
Goldilocks Would Love Incident Command
Incident Command structure should always be “just right” for the incident. It’s a modular system, not all-or-nothing!
Annual Review of Emergency Preparedness Plan
by Rick Christ Current CMS Emergency Preparedness Conditions of Participation require an annual review of your emergency preparedness plan. Under the proposed rule, the plan “must be evaluated and updated at least every 2 years.” Not in the rule, but in...
Why We Support More Detailed Exercise Standards
by Rick Christ Currently, almost every provider type is required to participate in two exercises per year. One “should be” a “community full-scale exercise” while the other can be a tabletop. The original version of the current exercise standards was...
Do the Proposed Changes to Training Make Sense?
by Rick Christ Currently, the typical CMS regulation says this about the training requirement: The training and testing program must be reviewed and updated at least annually. (1) Training program. The hospital must do all of the following:(i) Initial...
Documentation of Cooperation and Collaboration
What You Need to Know About the Proposed Rule Changes to CMS
by Rick Christ Barely ten months into the enforcement period of the Emergency Preparedness Conditions of Participation, the Centers for Medicare and Medicaid Services (CMS) is proposing some rule changes that would “reform Medicare regulations that are...
CMS Compliance Products & Services
[/et_pb_shop]
[/et_pb_shop]
[/et_pb_shop]
Our Newsletter
Remember, we will NEVER share your email address or SPAM you.
You may unsubscribe at any time.
Website design & development by Carbon Six Digital Marketing Agency







We'd Love to Hear Your Comments